
ST. GEORGE — Preliminary data show that the flu shot worked roughly one-third of the time this season, but when broken down by strain, the level of performance varied widely – as influenza outbreaks continued across the country for months.
Seasonal flu takes a heavy toll on Americans, and this year was particularly severe, largely due to the circulating flu strains, which are a mix of different strains of viruses. H3N2 commonly leads to more severe illness and a higher number of hospitalizations, according to the Centers for Disease Control.
The 2017-2018 flu season officially began Oct. 1, 2017, and the CDC’s most recent “Weekly U.S. Influenza Surveillance Report” released April 28 marked the 17th week.
The effectiveness of the flu vaccination came into question this year. According to David Heaton, Southwest Utah Public Health Department public information officer, the flu vaccine was 36 percent effective overall this season, based on calculations by the CDC using data collected since February. However, Heaton said, that percentage taken alone doesn’t represent the entire picture.
“On any given year, the typical effectiveness level of a good vaccine is around 60 percent,” Heaton said, “and while 36 percent is low, that really doesn’t tell the whole story.”
Being that the vaccine protects against three different viruses, he said, each with varying effectiveness rates, that number is derived from averaging out all three.
For example, the H3N2, a particularly “nasty virus,” had an effectiveness rate of 25 percent, Heaton said, while the H1N1 strain, or “Swine Flu” virus left over from the deadly pandemic in 2009, had a 67 percent effectiveness rate, a level that is above average.

The science behind vaccine development begins with testing flu strains coming out of the southern hemisphere that are present this year, he said, combined with strains that were present in the past.
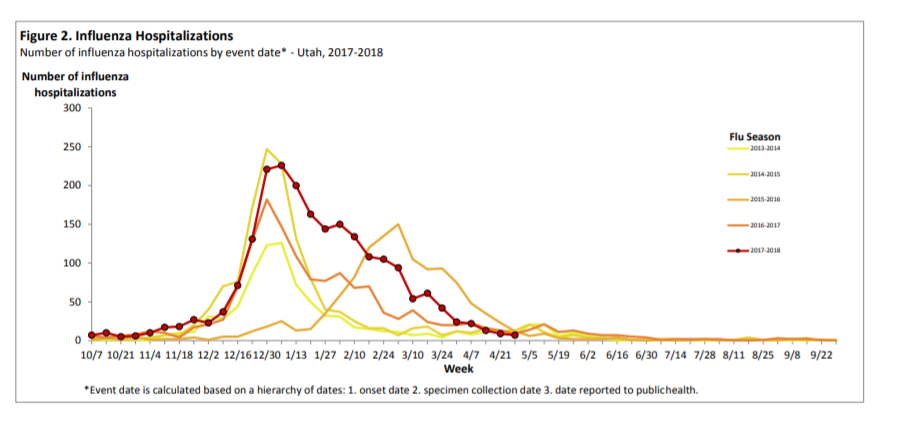
Since the flu season opened, 220 people have been hospitalized within the Southwest Region, an area covering Beaver, Kane, Iron, Garfield and Washington Counties, according to a Utah Department of Health weekly update report dated April 28.
By comparison, Salt Lake County had the highest number of hospitalizations, with 986 during the same reporting period.
Statewide, the report shows nearly 2,140 individuals have been hospitalized, compared to 1,470 during the 2016-2017 season, and the risk of hospitalization nearly tripled for those who are over the age of 65, according to the data.
More than half of those admitted with the flu were over the age of 65, and less than 375 were between the ages of 50-64, with children ages 0-4 representing the lowest number, with 159 cases.
In Utah, 288 people have died so far this season.
Flu season 2017-2018 in Nevada
The number of deaths reported for Clark County, Nevada, was updated to 47, after an increase in flu activity prompted the Southern Nevada Health District’s Office of Epidemiology and Disease Surveillance department to team up with other agencies to review and update previously reported cases of flu.
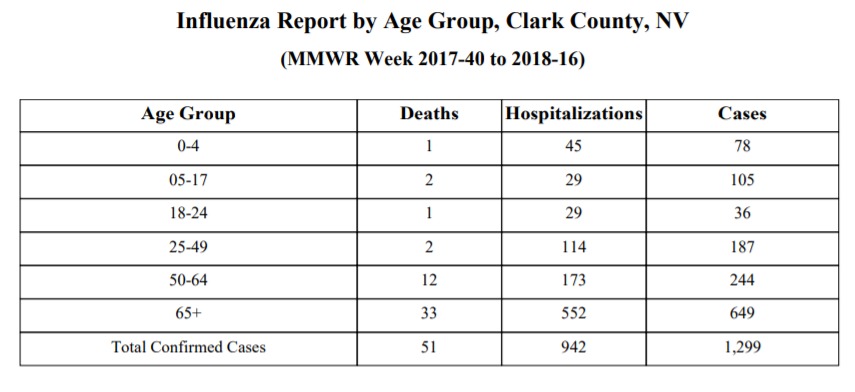
Additionally, flu cases reported in Nevada’s Southern District saw a sharp increase from 2017 to 2018, according to a report released April 28.
Last year, 612 flu cases were reported, with 422 hospitalizations and 13 deaths, while the number of cases so far this year has more than doubled, with nearly 1,300 cases reported during the 2017-2018 season as well as 942 hospitalizations.
The death toll for 2017-2018 season rose to 51, nearly four times higher than the preceding year.
The number of flu cases statewide saw a sharp hike as well, with more than 11,000 cases, up from 8,570 the previous season, according to a report released in February by the Nevada Department of Health and Human Services.
The CDC data show that 357 people have died from flu-related illnesses to date.
Flu season 2017-2018 in Arizona
Arizona’s numbers are even more remarkable, with more than 21,260 flu cases reported during the 2017-2018 flu season, up from 2,561 – which is more than 730 percent higher, according to an Arizona Department of Heath Influenza Summary 2017-2018 Flu Season report recently released.
Additionally, the death toll has nearly tripled, with 785 deaths in 2017-2018, compared to 239 deaths the prior year, according to a CDC “Fluview” report.
The report also shows that by the beginning of February, the number of confirmed flu cases in Arizona surpassed the total seen during the H1N1 flu pandemic of 2009-10, with nearly 19,300 reported cases.
High death toll in children
This flu season was particularly deadly for children, and those under the age of 2 were at the highest risk. The CDC reported April 27 that there have been 160 flu-related deaths among children so far, up from 101 reported during the 2016-2017 flu season, a death rate nearly 60 percent higher.
In past seasons, more than 80 percent of the children who died were not vaccinated that particular year, according to the CDC.
The April report also shows the highest number of pediatric deaths – 43, or one-quarter of all flu-related deaths – were reported in Region 4, which includes Alabama, Florida, Georgia, Kentucky, Mississippi, North Carolina, South Carolina and Tennessee.
Utah is in Region 8, which has one of the lowest number of pediatric deaths.
Since 2004, the first year the CDC began tracking flu-related deaths in children, the higher number of pediatric deaths is attributed to the H3N2 virus that dominated the influenza landscape this season, a strain that causes more severe symptoms, particularly in children.
The bigger picture
On average, the flu causes 30,000 deaths and 200,000 hospitalizations in the U.S., mostly among people 65 years or older, and this season 45 states declared widespread flu outbreaks, with severe levels reported across much of the country, according to the CDC.

Taking into account the vaccine carried a lower level of overall effectiveness, it still offers a higher level of protection than having no vaccine at all, Heaton said.
“We have thousands of usually older people who are hospitalized and die every year from the flu,” he said. “So, even with a lower level of protection, it will still prevent thousands of illnesses, hospitalizations and death.”
The CDC showed similar findings, and reported that even with the vaccine’s lower overall rate of effectiveness, much of the problem can still be prevented by an annual vaccination, which the agency states is proven safe and effective in combating seasonal flu.
In spite of this, vaccination rates among Americans remain low, and fewer than half of all persons were vaccinated against the flu in 2016. The age group with the lowest vaccination rate – 31 percent – are between 18 and 49 years of age. Further, less than half of all children were vaccinated during that period.
One factor that may influence the low vaccination numbers is the idea that the flu shot can cause the flu, which Heaton said is impossible.
Flu vaccines are made in such a way as to prevent infection. One way uses flu viruses that have been inactivated, so they are not infectious. Another is made using no flu viruses at all.
The most common side effects from the influenza shot are soreness, redness, tenderness or swelling where the shot was given. Low-grade fever, headache and muscle aches also may occur.
There is an additional agent that could cause an allergic reaction for those allergic to eggs, due to the fact that vaccines are produced by growing each individual dose of the vaccine inside of an egg, Heaton said, noting that the number of doses made is equal to the number of eggs used.
That may be changing in coming years, he added, as scientists are currently developing other mediums in which to grow the virus that wouldn’t include eggs.
Every year seasonal flu viruses cause substantial illness and death, much of which could be prevented. Health officials encourage everyone to get flu vaccinations, especially those at high risk of complications from the flu, including children younger than 5, adults age 65 and older and pregnant women. Children younger than 2 have the highest risk of developing complications from the flu.
It is especially important for people who are more susceptible to complications from flu get vaccinated, including those with chronic medical conditions like heart disease, diabetes, kidney disease or respiratory conditions. Anyone who care for babies younger than 2 months old should also be vaccinated.
According to the CDC, for the last 15 flu seasons, the average duration of a season has been 13 weeks, with possible ranges of one week to 20 weeks.
The week ending April 28 marked the 17th week for this year’s flu season, and it may not be over yet.
Email: [email protected]
Twitter: @STGnews
Copyright St. George News, SaintGeorgeUtah.com LLC, 2018, all rights reserved.