ST. GEORGE — Simulation mannequins, or SimMen, are improving the training of the Intermountain frontline medical staff in Southern Utah.
Sammy and Andy Mannequin live at the Learning Centers at Valley View Medical Center and Dixie Regional Medical Center and are subjected to rigorous procedures, intense situations, pokes, prodding and tests. They blink, lose the contents of their stomachs and even yell. Caregivers draw blood from their arms (albeit a very small amount) and assist as they give birth.
Valley View and Dixie Regional introduced Sammy and Andy in their education departments to provide dozens of lifelike training scenarios to clinical staff at the hospitals and in the community.
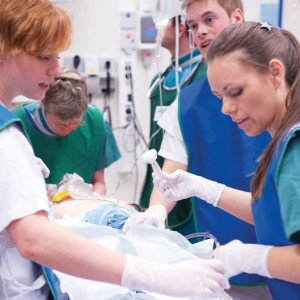
These high-tech mannequins allow for advanced, hands-on training because of their ability to simulate everything from a closed airway, to a heart attack, a belligerent patient or a stroke.
“We use Sammy and Andy to learn how to best do things like compressions, open airways and any and all lifesaving techniques,” said Brenda Seegmiller, education consultant at Valley View. “Even though the mannequins aren’t real people, it makes the experience as true to life as it can be.”
A control room with a one-way mirror sits next to the room where Sammy and Andy are kept, and a special computer is hooked up to them to carefully assess and monitor actions. The simulation facilitator sits behind the one-way mirror and, through a special microphone, can talk and even shout like a patient might through small speakers in the mannequins.
“We’ve had more than one hundred participants go through this simulation so far region-wide,” Seegmiller said. “If mistakes are made, Andy and Sammy aren’t real people. That’s the joy in a simulation program — rest assured that no one gets hurt in the learning process.”
The facilitator can open and shut the eyes, and mouths feature a realistic tongue and teeth, aiding in the realistic nature of providing lifesaving care. Unlike an actual patient, who might be unconscious or unaware of what lifesaving technique is being used, the mannequins feature hundreds of sensors that are able to record such things as how deep a chest compression was given and provide feedback to the student if they need to do more quick compressions or deeper compressions.
“Using Sammy and Andy is a fun way to learn and know that you’re doing it the right way,” Seegmiller said. “Each newly hired registered nurse who is being trained for the medical or surgical areas of the hospital will participate in nursing unit orientation simulation.”
Andy and Sammy’s significance at the hospital appears to be paying off for participants.
“We’ve had had such great feedback, especially from the nurse residents, that they’re able to recall what they learned from the simulations and so have known exactly what to do,” Becky Holt, who directs education for the Southwest Region of Intermountain Healthcare said, adding:
The situational simulations mimic real life. There have been some trauma simulations where we can intubate the mannequins, put chest tubes in or needle them for a pneumothorax (where air leaks into the space between your lungs and chest wall). The nurses and participants don’t have to be hesitant and can be more assertive in their learning.
Not all of the credit can be given to the SimMen.

“We have some great simulation facilitators who have all been trained by the corporate team to teach in our classroom,” Seegmiller said. “Facilitators have strict requirements to meet before being placed in a classroom with the mannequins. One of those is to attend a three-day training in Salt Lake, and it only happens a few times annually and space is limited, so we are lucky to have as many facilitators as we do.”
Combined, Dixie Regional and Valley View currently have 25 simulation facilitators and 14 neonatal resuscitation provider instructors, including four physicians.
“The three-day training is very intense. Several scenarios are ran, with everyone rotating between participant and facilitator,” Holt said. “We’re taught how to write scenarios so they can be understood by anyone, whether it be a nurse or a non-medical participant.”
Facilitators are even taught moulage tricks to make the simulations more realistic. Moulage is a French term for the art of applying mock injuries for the purpose of training emergency response teams and other medical and military personnel.
“It’s much more difficult than one would think to make props such as vomit!” Holt said. “We discovered that oatmeal, Parmesan cheese and lemon juice makes an awesome, smelly substitute. It takes practice and patience to create moulage, but we also have a lot of fun with it.”
Sammy and Andy aren’t the only mannequins who are making a difference. There’s Manny, who can get intubated, a SimBaby who can provide practice for pediatric emergency care and a SimMom who can simulate giving birth.
“We’re hoping to take SimMom on the road to teach nurses how to handle situations with mom and baby, both normal and not,” Seegmiller said. “Intermountain understands just how important these simulation mannequins are to training front-line staff and community members in emergency response and so have been working very hard to get more departments involved in trainings and to add more scenarios for simulation labs.”
Holt said the goal for the simulation program is to get more clinical nursing staff involved.
Local simulation programs will continue to assist and serve the community by creating safe and effective learning environments with the help of permanent residents Andy and Sammy.
“Our participants and nurses are getting a more intense training and practice so that in no matter what situation, they can provide the very best care for patients,” Seegmiller said. “It’s great for Intermountain to provide so many great resources for this type of learning. It has absolutely improved the level of training and lifesaving response in our area of the state. The simulation program is changing and saving lives.”
Written and submitted by Becki Bronson, Valley View Medical Center, Cedar City
Related posts
- Patient Safety Movement ranks Intermountain in Top 3 for eliminating preventable deaths
- Three doctors join Intermountain Medical Group
- Intermountain clinics introduce new oncologist, dermatologist
Email: [email protected]
Twitter: @STGnews